In late 2021, the Food and Drug Administration approved a drug that protects immunocompromised patients from COVID-19 and succeeds where traditional vaccines had failed.
But there’s a catch. Receiving the shot can cost more than $1,000, even though the federal government agreed to purchase more than a million shots and give them to hospitals for free.
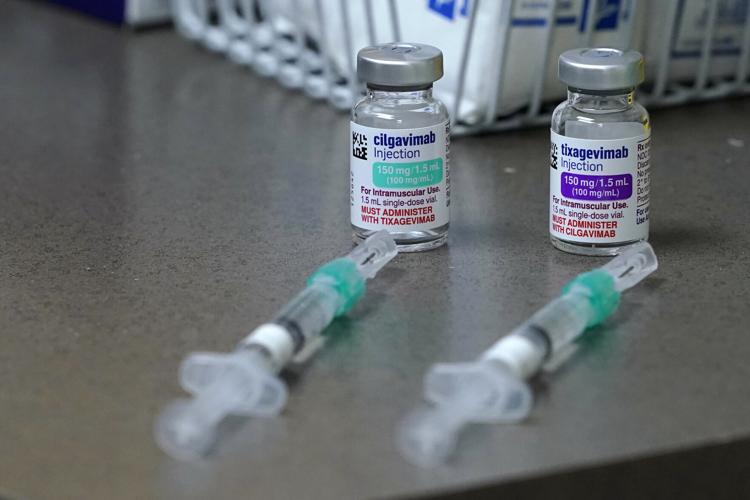
Patients with immunocompromising conditions, such as organ transplants and cancer, often receive little or no boost from traditional vaccines. But a drug called Evusheld protects these patients from developing infection.
While healthy patients can receive COVID vaccines for free, Virginia Commonwealth University Health and University of Virginia Health charge more than $1,000 for the administration of Evusheld. What a patient actually pays out of pocket depends on insurance.
People are also reading…
One organ transplant recipient who lives in Charlottesville got her shot at UVA. While her insurance covered most of the expense, she was left with a bill of $296.
These aren’t one-time costs, either. The FDA recommends immunocompromised patients receive Evusheld every six months. The expense is likely a reason why so few immunocompromised people have taken the medicine, and that leaves them feeling neglected.
“It’s been extremely frustrating,” said a Southwest Virginia kidney transplant recipient. “Those who have chosen to fight for their survival have been forgotten and abandoned.”
Hospitals aren't the only facility charging for it. The Virginia Cancer Institute in Mechanicsville charges an administrative fee, but what a patient pays out of pocket depends on insurance, said Shonda Clements, a nurse there.
Stephanie DeNicola, 44, of Charlottesville is one of about 7 million Americans living with an immunocompromising condition.
She has rheumatoid arthritis, and her medication, methotrexate, acts like a chemotherapy, dampening her immune system. She’s more susceptible to ordinary viruses and bacteria, such as E. coli, which she said almost killed her.
“Anything can kill me,” DeNicola said. “COVID is just the latest thing that can kill me.”
Vaccines have limited or no effect on her and, when she received her first COVID shot, her antibody level was one-one-thousandth that of a healthy recipient, she said. By the time she got her third shot, she had one-tenth as many antibodies as a healthy patient.
But Evusheld offered a glimmer of hope in a way vaccines had not. The AstraZeneca-made drug is a monoclonal antibody designed for people not infected with COVID who can’t mount an adequate immune response. It received its emergency-use authorization in December and, in trials, it reduced the risk of COVID infection by 77%.
While health care facilities have plenty of shots, uptake has been low. Only 165,000 have been delivered as of last month, a Health and Human Services official said. Many people still don’t know about the medicine.
Others are choosing to pay whatever it costs to gain protection. Leanne Cook, a resident of Orange County, Calif., said she paid $1,300 for Evusheld through her high-deductible plan with Aetna. Her next dose is scheduled soon. Because she’s already paid her out-of-pocket maximum, the next round should be free.
UVA Health doesn’t charge for Evusheld itself, but it does charge to administer it, a process that includes monitoring the patient for an hour after injection. UVA charges insurance companies between $149 and $1,190.
Asked why UVA asks for so much, a spokesperson said the health system set the price based on administrative charges for similar medications. Administrative charges reflect substantial time for preparation, delivery and post-injection monitoring.
VCU’s gross charge for Evusheld administration is $1,400, according to a spokesperson for the health system. A gross charge is the price before a hospital negotiates a lower rate with an insurer.
VCU Health aims to “lead the nation in quality, affordability and impact as a trusted and preferred academic health system,” the spokesperson said. “As such, we are committed to empowering patients and their families to make informed decisions about their health care.”
HCA Healthcare doesn’t offer Evusheld, a spokesperson said. Bon Secours does not charge for it, a spokesperson for the health system said.
While the federal government decided health care facilities can’t charge for COVID vaccine administration, it didn’t make the same decree for Evusheld.
“It’s outright discrimination that the immunocompromised are required to pay and those who are immunocompetent are not,” said the Charlottesville woman who paid $296 for her shot from UVA. The woman, who received a kidney transplant, requested anonymity because she fears speaking out could impact her ability to receive another kidney later in life.
The Southwest Virginia kidney recipient also opted to get Evusheld, even though he didn’t know how much it would cost him until he got his bill. It felt like signing a blank check, he said. Ultimately, his insurance covered the entire cost. He also requested anonymity.
DeNicola didn’t have to pay, either. Her Elevance Health (formerly Anthem) insurance plan covered the entire cost.
In Virginia, the state health department does not have the authority to set caps on administrative costs, a spokesperson for the department said. It doesn’t monitor which facilities charge and which do not.
Immunocompromised people are essentially left to protect themselves, the Charlottesville woman said. At the very least, eliminating administrative fees for Evusheld would put “us on an even keel with everyone who’s immunocompetent,” she said.

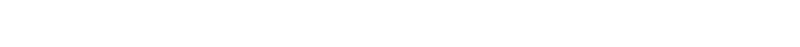














![A1 Minute! March April 17, 2024: Warm temperatures continue; Branch Building purchased by Ashley Williams; Brown’s Island gets upgrade[A1]](https://bloximages.newyork1.vip.townnews.com/richmond.com/content/tncms/assets/v3/editorial/0/a7/0a705b54-eb55-5b79-88ae-c3a4a91f6e8d/661fe40b3eeb2.image.jpg?resize=150%2C84)